

A study by the University of Illinois Chicago has discovered a mechanism behind cognitive impairments in mice with COVID-19 and tested a gene therapy that improves symptoms. Focusing on the blood-brain barrier and a specific signaling pathway, the research offers a hopeful avenue for preventing post-COVID-19 cognitive issues in humans by enhancing barrier integrity.
Memory loss and learning difficulties are among the many confounding symptoms observed in individuals recovering from COVID-19. Yet little is known about the mechanisms of cognitive impairments like these, commonly called brain fog.
In a new study, researchers at the University of Illinois Chicago have identified a mechanism that causes neurological problems in mice infected with SARS-CoV-2, the virus behind COVID-19. The researchers also found a treatment that helped prevent these changes. Sarah Lutz, assistant professor of anatomy and cell biology in the College of Medicine, led the research, which was published in the journal Brain.
The team focused on the blood-brain barrier, which plays a role in other neurological diseases, such as multiple sclerosis. Normally, this barrier protects the brain from potentially harmful cells or molecules circulating in the bloodstream. But the infected mice, researchers found, had leaky blood-brain barrier vessels and impaired memory or learning.
To understand why, the researchers looked at blood vessels from the brains of infected mice to see which genes were most altered. They found a significant decrease in a signaling pathway called Wnt/beta-catenin, which helps maintain the health of the blood-brain barrier and protects the brain from damage.
Promising Gene Therapy Findings
With these results, the team explored whether a gene therapy that stimulates the Wnt/beta-catenin pathway could prevent brain damage in mice who were infected with SARS-CoV-2.
Indeed, it did just that.
“They had less blood-brain barrier leakage and less immune cell infiltration of the brain, which led to improvements in learning and memory,” Lutz said.
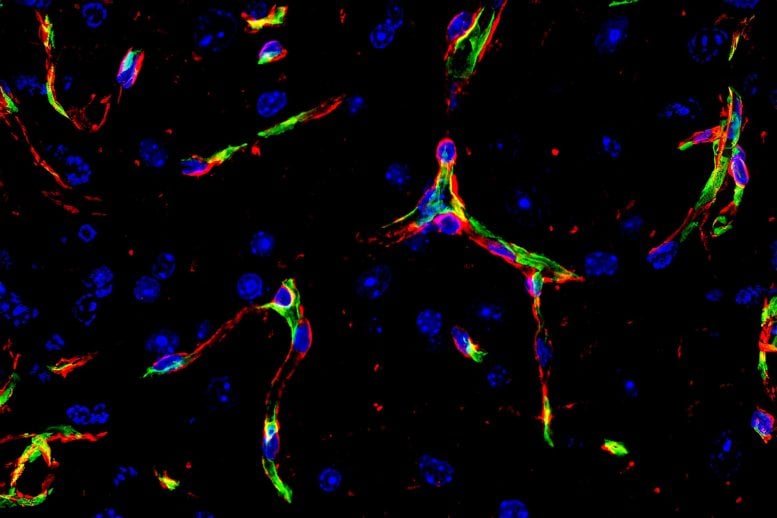
Blood vessel endothelial cells (green) and basement membrane (red) in the brain. Credit: Sarah Lutz
Because age is a risk factor for cognitive impairment in humans with COVID-19, the team focused on older mice in their research. They specifically tracked mild infections in the mice. Mild, rather than severe, infections account for most COVID-19 cases in humans today, thanks to the vaccine. Yet even mild infections can cause cognitive impairment, Lutz said.
While the research is a long way from establishing a therapy for humans to prevent post-infection cognitive impairments, this study is an important step on that path, Lutz said.
“Anytime you can identify a molecular mechanism that contributes to a disease, you’re learning about basic biology and what causes disease in general,” she said. “This research suggests that improving blood-brain barrier integrity could have benefits in preventing complications of COVID-19.”
One major lesson from the COVID-19 pandemic is that even mild infections can profoundly affect organs, including the brain, explained Dr. Jalees Rehman, the Benjamin Goldberg Professor and head of the UIC Department of Biochemistry and Molecular Genetics and a co-author on the study.
“There is a need for more research on respiratory infections that can affect the brain,” Rehman said. “The good news is that by studying the molecular signals activated by the infection as well as during the subsequent inflammation when the immune system responds to infection, one can develop new targeted therapies which prevent further damage to the brain and other organs.”
Reference: “Engineered Wnt7a ligands rescue blood–brain barrier and cognitive deficits in a COVID-19 mouse model” by Troy N Trevino, Avital B Fogel, Guliz Otkiran, Seshadri B Niladhuri, Mark A Sanborn, Jacob Class, Ali A Almousawi, Benoit Vanhollebeke, Leon M Tai, Jalees Rehman, Justin M Richner and Sarah E Lutz, 02 February 2024, Brain.
DOI: 10.1093/brain/awae031
The study was funded by the National Institutes of Health and the University of Illinois Institutional Funds.